I. How to Use
When to Use
Use the dosing calculator during procedures involving higher doses of local anesthetics (i.e. nerve blocks, regional anesthesia) to reduce risk of toxicity and adverse effects including local anesthetic systemic toxicity (LAST).
Pearls / Pitfalls
-
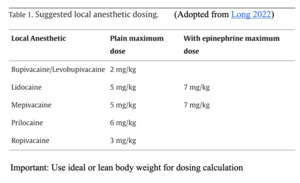
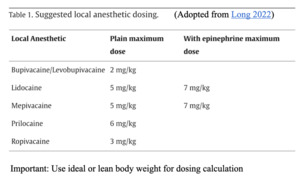
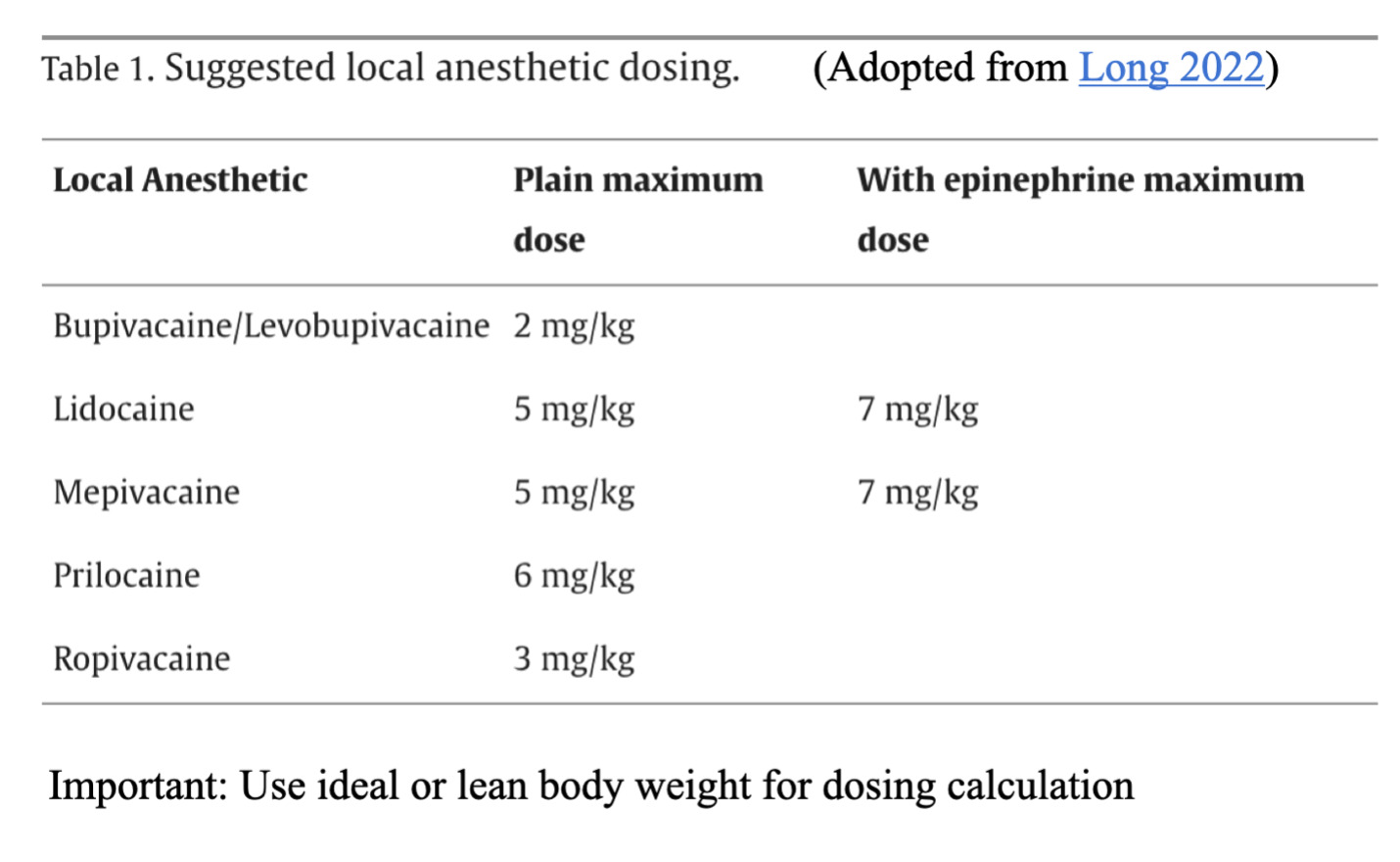
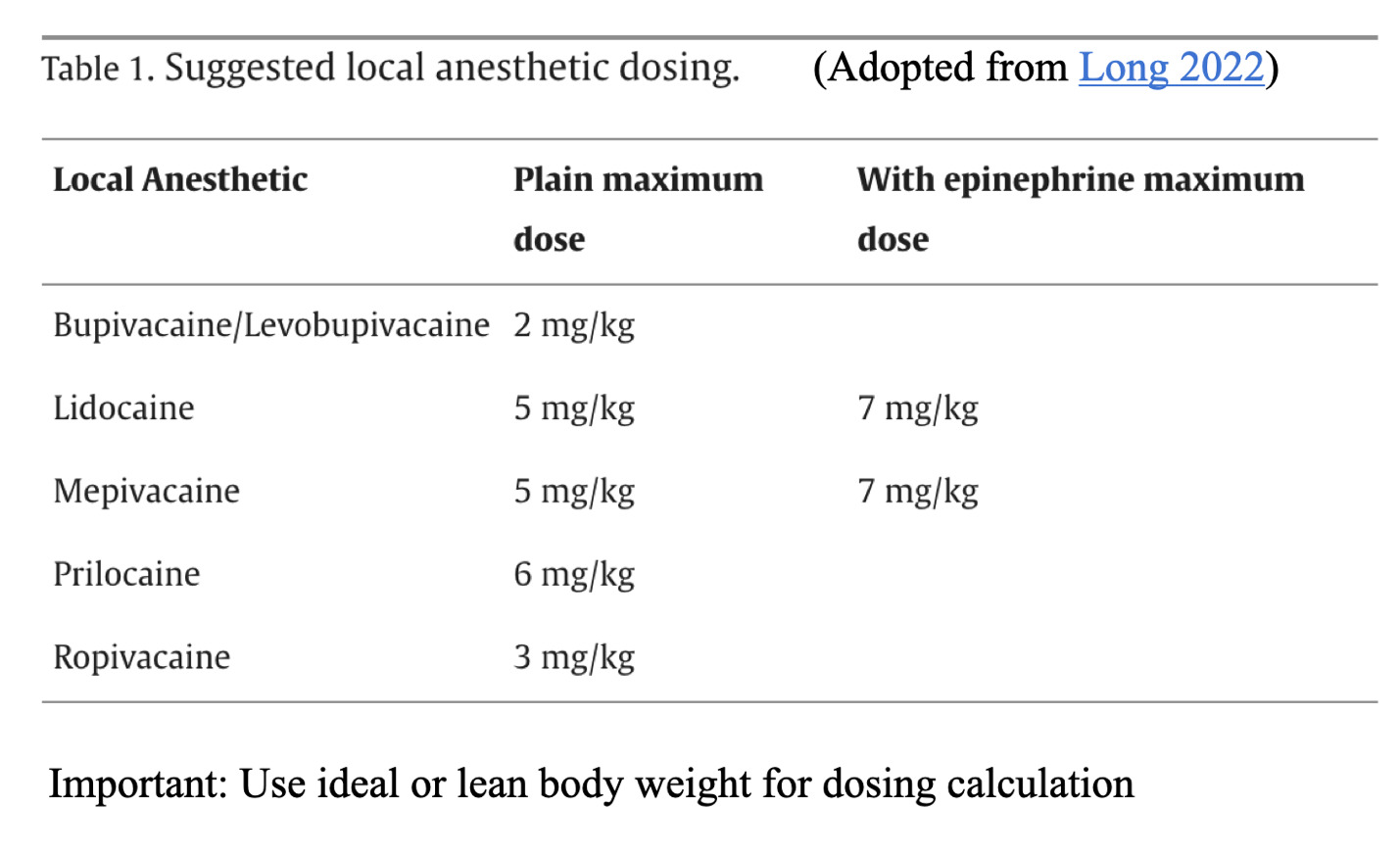
The anesthetic toxic dose is based on ideal body weight.
-
Local anesthetic systemic toxicity (LAST) is rare but potentially life-threatening. Symptoms can be divided into two main categories:
-
Neurotoxicity: perioral numbness, metallic taste, mental status changes or anxiety, visual changes, muscle twitching, and ultimately, seizures, coma, and respiratory depression.
-
Cardiovascular toxicity: tachycardia, hypertension, ventricular arrhythmias, and/or asystole.
-
Patient risk factors for LAST include:
-
Extremes of age.
-
Decreased muscle mass.
-
Renal, hepatic, or cardiac disease.
-
Metabolic disturbances (acidosis, hypoxia, hypercarbia).
-
Pregnancy.
-
-
Procedural risk factors for LAST include:
-
Injection into highly vascular areas (highest incidence in paravertebral injections, followed by upper and lower extremity peripheral nerve blocks).
-
Large laceration repairs and intradermal injections.
-
Multiple injections or continuous infusion.
-
-
Ways to reduce the risk of LAST (Bailey 2025, On’Gele 2024):
-
Calculate the patient’s maximum dose.
-
Dilution of anesthetic with normal saline allows for larger volume blocks to be performed without risking toxic doses.
-
Vasoconstrictors, such as epinephrine, can be added to decrease rate of absorption and therefore decrease toxic dose.
-
Use ultrasound to confirm needle placement.
-
Aspirate prior to injecting.
-
Perform a slow injection and look for appropriate anesthetic spread when using ultrasound guidance.
-
Monitor for development of symptoms.
-
Why Use
It is important to appropriately dose local anesthetics and reduce the risk of LAST by calculating the maximum dose in advance to reduce risk.
II. Next Steps
Advice
-
If the anesthetic dose is above the threshold for toxicity, consider lowering the dosage to the weight-determined range.
-
Prepare for adverse events by having a nerve block checklist and having intralipid readily available and easy to access.
Management
LAST is an uncommon but potentially life-threatening complication of local anesthetic use that may be encountered in the ED, hospital, or surgical center. Patients at extremes of age or with organ dysfunction are at higher risk. Inadvertent intra-arterial or intravenous injection, as well as repeated doses and higher doses of local anesthetics are associated with greater risk of developing LAST. Using ultrasound guidance, aspirating prior to injection, and utilizing the minimal local anesthetic dose needed are techniques that can reduce the risk of LAST.
Diagnosing LAST
Local anesthetic toxicity results from sodium channel blockade, which affects the central nervous system and cardiac system. The CNS is more sensitive to the effects of local anesthetics than the cardiac system and will generally manifest signs/symptoms of toxicity first.
The presenting symptoms of LAST include perioral numbness, metallic taste, mental status changes or anxiety, visual changes, muscle twitching, and ultimately, seizures, coma, and respiratory depression. Cardiovascular effects include tachycardia, hypertension, ventricular arrhythmias and/or asystole.
Management of LAST: (see guidelines: American Society of Regional Anesthesia and Pain Medicine Local Anesthetic Systemic Toxicity checklist: 2020 version)
Management of LAST requires immediate recognition and a coordinated response, starting with stopping the local anesthetic administration and calling for expert help while initiating a dedicated LAST protocol. Prioritize airway management, airway support with 100% oxygen or noninvasive ventilation, and support circulation according to advanced cardiac life support (ACLS) guidelines. Crucially, avoid calcium channel blockers, beta-blockers, and lidocaine, as they can worsen cardiovascular depression and toxicity; use epinephrine in smaller doses (< 1 mcg/kg) for LAST-induced shock. Seizures should be promptly controlled with benzodiazepines (e.g., midazolam, lorazepam), avoiding propofol which can exacerbate cardiovascular depression. For cardiovascular compromise, including hypotension and life-threatening arrhythmias, 20% lipid emulsion therapy is critical: administer an initial bolus (e.g., 1.5 mL/kg over 1 minute) followed by a continuous infusion (e.g., 0.25 mL/kg/min). Repeat boluses can be given after 5 minutes for 2 or more times for persistent hemodynamic instability. Vigorous resuscitation should continue until stability is achieved, followed by close monitoring in an intensive care setting.
Critical Actions
Multiple variables may influence a patient’s risk of developing LAST. This weight-based calculator should be used to generate a rough estimate for toxic doses.
III. Evidence
FORMULA
Max allowable subQ dose based on ideal body weight, mg = max allowable subQ dose for a drug, mg/kg × weight, kg
Max allowable subQ dose based on ideal body weight, mL = max allowable subQ dose for a drug, mg/kg × (weight, kg / 10) × (1 / concentration, %)
Evidence Appraisal
There are no randomized clinical trials involving LAST. Much of the existing evidence is based on case reports, expert opinion, and retrospective anesthesia databases.
Original/Primary & Validation
- Sztajnkrycer MD. Local Anesthetics. In: Hoffman RS, Howland M, Lewin NA, Nelson LS, Goldfrank LR. eds. Goldfrank’s Toxicologic Emergencies, 11e New York, NY: McGraw-Hill; 2019.
Clinical Practice Guidelines
-
AAGBI Safety Guideline. Management of Severe Local Anaesthetic Toxicity. https://anaesthetists.org/Home/Resources-publications/Guidelines/Archived-guidelines/Management-of-severe-local-anaesthetic-toxicity
-
Neal JM, Barrington MJ, Fettiplace MR, et al. The Third American Society of Regional Anesthesia and Pain Medicine Practice Advisory on Local Anesthetic Systemic Toxicity: Executive Summary 2017. Reg Anesth Pain Med. 2018;43(2):113-123.
-
Lavonas EJ, Akpunonu PD, Arens AM, Babu KM, Cao D, Hoffman RS, Hoyte CO, Mazer-Amirshahi ME, Stolbach A, St-Onge M, Thompson TM, Wang GS, Hoover AV, Drennan IR; American Heart Association. 2023 American Heart Association Focused Update on the Management of Patients With Cardiac Arrest or Life-Threatening Toxicity Due to Poisoning: An Update to the American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation. 2023 Oct 17;148(16):e149-e184. doi: 10.1161/CIR.0000000000001161.
Other References
-
Schwartz DR, Kaufman B. Local Anesthetics. In: Hoffman RS, Howland M, Lewin NA, Nelson LS, Goldfrank LR. eds. Goldfrank’s Toxicologic Emergencies, 10e. McGraw-Hill Education; 2015.
-
Rosenberg PH, Veering BT, Urmey WF. Maximum recommended doses of local anesthetics: a multifactorial concept. Reg Anesth Pain Med. 2004 Nov-Dec;29(6):564-75; discussion 524. doi: 10.1016/j.rapm.2004.08.003. PMID: 15635516.
-
Miller’s Anesthesia: Local Anesthesia: 10th Edition, chapter 25: Gropper, M. A., Cohen, N. H., Eriksson, L. I., Fleisher, L. A., Leslie, K., & Johnson-Akeju, O. (Eds.). (2025). Local anesthetics (Chap. 25, p742-767) in Miller’s anesthesia (10th ed.). Elsevier.
-
Bailey JG, Barry G, Volk T. Local anesthetic dosing for fascial plane blocks to avoid systemic toxicity: a narrative review. Can J Anaesth. 2025;72(9):1423-1447.
-
On’Gele MO, Weintraub S, Qi V, Kim J. Local Anesthetics, Local Anesthetic Systemic Toxicity (LAST), and Liposomal Bupivacaine. Anesthesiol Clin. 2024 Jun;42(2):303-315. doi: 10.1016/j.anclin.2023.11.011.
-
Neal JM, Neal EJ, Weinberg GL. American Society of Regional Anesthesia and Pain Medicine Local Anesthetic Systemic Toxicity checklist: 2020 version. Reg Anesth Pain Med. 2021 Jan;46(1):81-82. doi: 10.1136/rapm-2020-101986.
-
Long B, Chavez S, Gottlieb M, Montrief T, Brady WJ. Local anesthetic systemic toxicity: A narrative review for emergency clinicians. Am J Emerg Med. 2022 Sep;59:42-48. doi: 10.1016/j.ajem.2022.06.017